More than 3,000 children are born every year with a congenital limb deficiency in the United States alone. These children will change their prosthetics devices once every 6 months, making the purchase of a high-end prosthesis unaffordable for most families. Affordable 3D printers have spawned numerous customizable and very affordable prosthetic hand models. These devices can be modified to fit the children as they grow, at a relatively low price. However, these prosthetic hands leave a lot to be desired in terms of functionality. Most of these devices can only allow coarse finger control, placing it in stark contrast to commercial automatic hands. The Project Sparthan team is committed to taking the concept of modular prosthetics a step further, continuing to bridge the gap between expensive robotic arms and 3D printed prosthesis. This will be done through the design and development of Sparthan, a modular electronics kit, compatible with existing prosthetic hand models, which will enable intuitive hand control.
Track: Hardware for Good
Fractal: Acoustic detection and monitoring of bone fractures
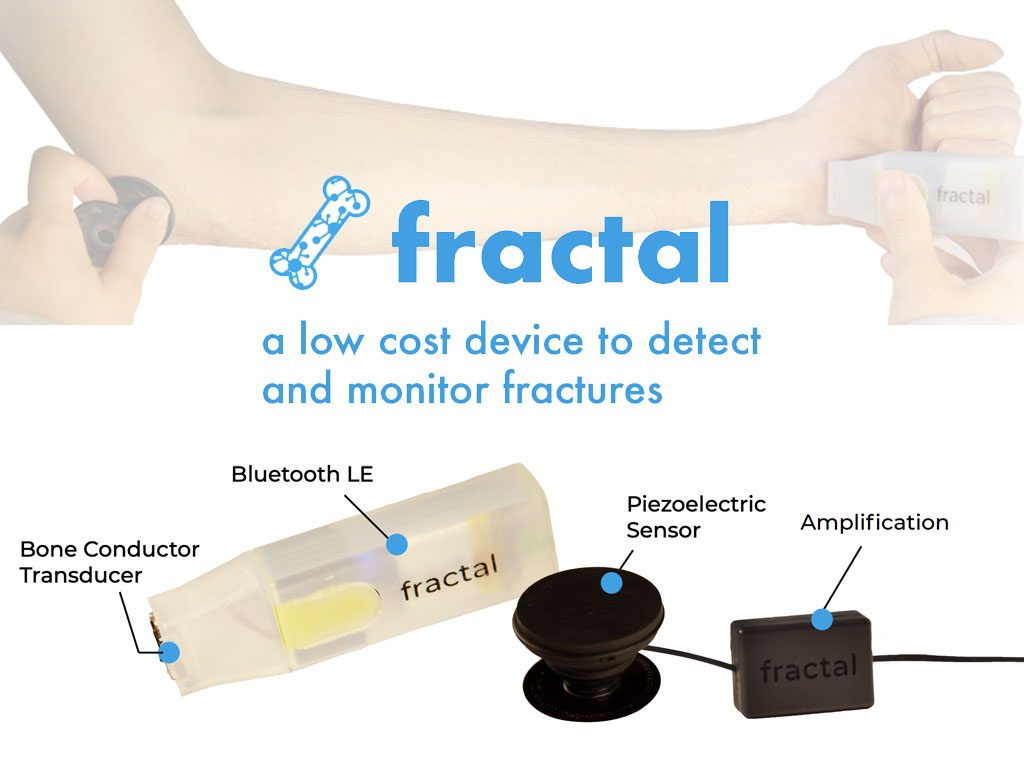
Two-thirds of the world lacks access to basic medical imaging equipment, which is an essential cornerstone for modern medical diagnostics. Due in part to a lack of access to basic x-ray technology in two-thirds of the world, fractures often mean a lifelong disability with devastating socioeconomic complications. In order to mitigate this gap in healthcare, Fractal provides underdeveloped countries and remote settings with an inexpensive, trusted tool for diagnosing and monitoring bone fractures. Fractal sends an acoustic signal through the bone, which is analyzed for sound transmission and frequency changes. The device is currently being tested on patients at the University of California, San Francisco with the aim to facilitate better care and outcomes for patients with plans for further development.
Sonic Eyewear Project

1.3 million people suffered from blindness in America in 2010 and that number is expected to triple by 2050. Many blind people click with their tongue as a means of soliciting echos from the environment which are processed by their brain and used to locate objects and navigate. While it has been shown to be extremely effective, the technique is difficult to master. The optimal clicking frequency is a critical part of the technique and is a challenge for many to learn. Sonic Eyewear looks like a regular pair of sunglasses that automates the clicking process by generating the optimal frequency of clicks on-demand. It sends forward-looking directional clicks when the user lightly taps her jaw to activate the signal. The technology leverages the power of the human brain to perform echolocation, which competitors have failed to do.
Isochoric Organ Preservation System: A Thermodynamic Approach to Saving Lives
Of the over 114,000 patients in the United States on the national transplant list, twenty die every day while waiting for an organ transplant, and every ten minutes another patient is added. Due to shortcomings in current organ preservation techniques, transplantation is prohibitively expensive, limited geographically to areas with large donor pools, and incredibly inefficient. This is driven by the short window of viability of organs after removal, on the order of four to six hours for hearts and lungs. Extending this viability from a few hours to a few days could transform the accessibility and affordability of organ transplantation, and could prevent up to 30% of all deaths in the US. The team has developed a novel solid-state device based on emergent thermodynamic principles. The isochoric cryopreservation chamber is capable of preserving live organs for long periods of time, which the team believes has the potential to transform the modern medical industry.
Respira Labs
Today, Chronic Obstructive Pulmonary Disease (COPD) affects 25 million Americans and costs the healthcare system nearly $50 billion a year. Respira Labs’ COPD management platform is based on a novel technology which instead of merely listening for changes in breathing like other wearable tools, emits sound from small sensors to capture personalized lung volume profiles based on resonance. This allows the technology to detect air trappings (abnormal increase in volume of residual air in the lungs after exhalation) which signals an exacerbation. Intelligent algorithms will flag patients in danger of readmission before acute symptoms arise, enable home-based intervention, cut hospital readmission costs, and reduce provider and payer healthcare bills. Initial customers will include heads of telemedicine who run hospital remote patient monitoring systems and who will champion adoption of the Respira Labs solution. Platform users are primary care physicians, pulmonologists, nurse practitioners, respiratory therapists, and post-hospital discharge COPD patients.
AsphyxiAlert

AsphyxiAlert addresses the need for a tracheostomy alarm system that alerts caregivers in the event of accidental tube dislodgement and tube occlusion. AsphyxiAlert’s dual purpose device houses sensing technology to warn against these two emergencies, with the ability to add extra features for the home consumer. In the case of airway compromise due to a tube dislodgement or blockage, the device will remotely display critical warnings to a personal electronic device or nursing station module. Using big data, the team will tailor the algorithm for each patient’s breathing to personalize the system. This safety device is for home and hospital/rehab facility use in both children and adults. While saving lives is AsphyxiAlert’s primary goal, this device can prevent costly hospitalization, consumption of resources and provide an early warning system as an FDA approved medical device.
QuickStitch Surgical
Suturing is a low-complexity yet technical and time-intensive step of every open surgical procedure. In recent years, few innovations in wound closure have worked to improve the process of closing open incisions. The QuickStitch device takes an innovative approach to enhancing the efficiency of the hand-suturing process, which is considered the gold standard in wound closure. By automating the delivery of the needle through the tissue, the tying of the surgical knot, and the cutting of the suture tail, QuickStitch helps save precious and costly OR time by accelerating and simplifying the wound closure process. The device can be utilized in the closure of any layer of tissue and promises the same quality of wound closure outcomes as hand-suturing. Most importantly, QuickStitch will decrease time spent suturing by more than 75% and therefore will reduce patient risk by decreasing time spent under anesthesia.
VIDI
Every patient’s nightmare is putting one’s health at risk by receiving a failed surgery. In the US, medical errors kill more than 200,000 patients per year, making it the third-leading cause of death. The avoidable morbidity is partially due to lack of vigilance from manual counting and tracking of surgical instruments. Time-consuming and error-prone, the current tracking procedures jeopardize patient safety by replacing time that should be spent on patient care with time accounting for surgical instruments. VIDI builds smart systems that leverage computer vision to increase hospital workflow efficiency and minimize medical errors by tracking the full spectrum of surgical tools, enhancing inter-department and multi-room collaboration, and seamlessly generating documentation and analyses for hospital staff.
Innovis Medical
Trauma disrupts every person’s blood clotting ability to stop bleeding and remains the second leading cause of preventable death in industrialized countries. With no effective medical device to provide physicians with full blood clotting data at the site of injury, medics resort to blind dosing that carries significant risk of internal blood clotting or having no effect altogether. While deployed, injured soldiers may not receive proper treatment for up to 24 hours. In the civilian sector, patient treatment may be delayed up to 3 hours before the data can be obtained at a hospital. At Innovis Medical, the team provides health care practitioners with the tools they need to diagnose clotting dysfunction at the point-of-care with a solid-state, disposable sensor capable of operating in mobile situations.